He kōrero mō mātou
BODE³ is an HRC-funded programme, funded from 2010-2015 and renewed for 2016-2021. Its goal is to estimate health and wider societal gains, costs, cost-effectiveness and equity impacts of health sector interventions, and build capacity in modelling of health sector interventions. There is also MBIE-funded BODE³ from 2014-2020.
- About BODE³, 2016-2021
- About BODE³, 2010-2015
- About MBIE-funded BODE³, 2014-2020
- Overview of funded "programmes" within BODE³
BODE³ 2016-2021
Objectives:
- To estimate the health gains (total & equity-related), costs and cost-effectiveness of dietary and physical activity interventions.
- To estimate the health gains (total & equity-related), costs and cost-effectiveness of interventions targeted by absolute risk of cardiovascular disease.
- To estimate which preventive interventions maximally: gain health among working age adults; increase productivity and decrease welfare payments; increase quality of life among older people.
How we do this:
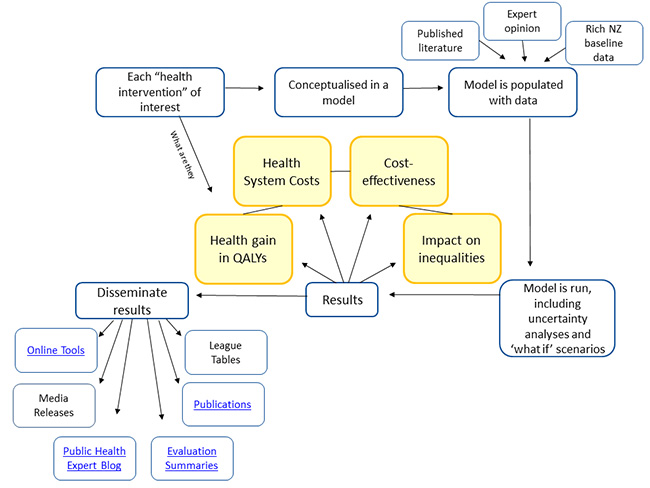
We are closely integrated with these NZ projects:
| The New Zealand Census Mortality and CancerTrends Study |
| DIET Programme (hosted by University of Auckland) |
| The Healthier Lives Challenge - He Oranga Hauora |
| The Virtual Health Information Network |
We collaborate with a range of research teams:
| PREDICT/VIEW | University of Auckland |
| Centre for Health Policy | Melbourne University (Prof Phillip Clarke, Dr Linda Cobiac and colleagues) |
| Nuffield Department of Population Health | Oxford University (Dr Peter Scarborough and colleagues) |
| Centre for Diet and Activity Research | Cambridge University (Dr Woodcock, Dr Mytton and colleagues) |
| Institute of Health Policy and Research | Erasmus University (Dr Pieter van Baal) |
Overview of the funded "programmes" within BODE³
 Health Research Council of NZ Programme Grant funding for BODE³:
Health Research Council of NZ Programme Grant funding for BODE³:
- 2016-2021: Focusing on preventive interventions (diet, physical activity, interventions targeted by level of cardiovascular disease risk) and morbidity and productivity costs around the retirement age
- 2010-2015: Focused on cancer control and preventive interventions, and capacity building
Health Research Council of NZ Programme Grant funding for the University of Auckland hosted DIET Programme, specifically:
- Objective 2: A Virtual Supermarket experiment of price variations in foods to generate improved price elasticities for modelling food taxes and subsidies
- Objective 5: Health gain and cost modelling of front of pack food labelling (randomised trial in Objective 1 of this DIET Programme), food reformulation (Objective 3 of this DIET Programme) and food price interventions (i.e. Objective 2 above)
Ministry of Business Innovation and Employment programme funding, 2014-2020, focusing on:
- 2014-16: Rapid assessment of multiple interventions
- 2016-19: In-depth research to improve quality of parameters identified in the initial modelling that cause large uncertainty in QALYs gained or cost outputs
- 2019-20: Update of modelling, with improved input parameters from in-depth research
CONTACT US
BODE³ Programme
Department of Public Health
University of Otago, Wellington
PO Box 7343
Wellington South 6242
New Zealand
Tel +64 4 918 5072
Email bode3@otago.ac.nz

