Pneumonia
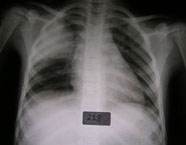 We have extensive experience in the clinical, diagnostic and epidemiological aspects of both adult and childhood pneumonia in a variety of settings. Our active involvement in clinical services places us in an ideal position to conduct both observational studies and clinical trials.
We have extensive experience in the clinical, diagnostic and epidemiological aspects of both adult and childhood pneumonia in a variety of settings. Our active involvement in clinical services places us in an ideal position to conduct both observational studies and clinical trials.
Important contributions of the Group include the development of the CURB65 severity assessment tool, documentation of ethnic differences in the incidence of pneumonia, and demonstration of Legionella and viruses as important causes of pneumonia.
In addition, Professor David Murdoch is a lead investigator on the Pneumonia Etiology Research for Child Health (PERCH) project, the world's largest pneumonia study, funded by the Bill and Melinda Gates Foundation.
Legionnaires' disease
 Pneumonia caused by Legionella bacteria (Legionnaires' disease) is a notifiable disease of public health importance.
Pneumonia caused by Legionella bacteria (Legionnaires' disease) is a notifiable disease of public health importance.
New Zealand has the highest reported incidence of Legionnaires' disease in the world, and our research has documented the high burden of this disease and the importance of sporadic (non-outbreak) disease and species other than Legionella pneumophila.
Our current focus is on the smart use of rapid diagnostics for Legionnaires' disease and identification of practical measures to prevent the disease.
Vitamin D
Vitamin D has been shown to be important for immune system function by enhancing and modulating the response to infection. We are interested in whether vitamin D has a role in the prevention or treatment of respiratory infections.
Invasive bacterial infections
 The Infection Group has had a long interest in staphylococcal disease, endocarditis, and vaccine-preventable invasive bacterial infections.
The Infection Group has had a long interest in staphylococcal disease, endocarditis, and vaccine-preventable invasive bacterial infections.
We have contributed to several Staphylococcus aureus databases and have had leadership roles within the International Collaboration on Endocarditis (ICE), the world's largest endocarditis database. We are also studying the transmission of S. aureus in schools and between humans and animals in rural communities.
We have also been actively involved in invasive bacterial infection surveillance in children in Nepal since 2005, in collaboration with Patan Academy of Health Sciences, the University of Oxford, and the World Health Organization.
Influenza
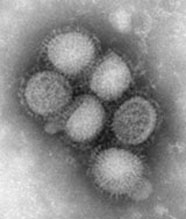
Globally, influenza continues to be responsible for a considerable burden of disease and hospitalisation every year.
Work lead by Associate Professor Lance Jennings has focused on evaluation and implementation of novel diagnostic tests, sentinel site surveillance, and pandemic preparedness.
Breath research
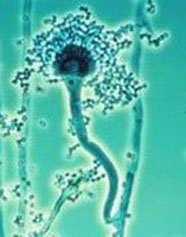 Our Breath Research Laboratory uses non-invasive breath tests to detect infectious lung pathogens.
Our Breath Research Laboratory uses non-invasive breath tests to detect infectious lung pathogens.
When micro-organisms grow they release volatile compound, these “volatiles” are normally non-specific, common to many species and therefore of very little value for diagnostic purposes.
Currently our group is working on the development of breath tests to detect Aspergillus fumigatus, Pseudomonas aeruginosa, Mycobacterium tuberculosis and Legionella infections.
The non-invasive nature of breath sampling means that it can be repeated and performed by small children with ease and thus may be particularly applicable to paediatric populations with minimal social impact.
Antimicrobials
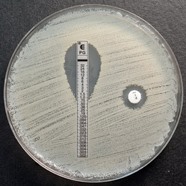 The ongoing emergence of antibiotic-resistant bacteria is a global concern.
The ongoing emergence of antibiotic-resistant bacteria is a global concern.
Our major strategic focus has been on defining pharmacokinetic and pharmocodynamic relationships of intravenous and oral antimicrobial dosing regimens in both the acute hospital setting and in outpatients settings in order to optimise clinical outcomes.
These activities complement the implementation of an active antimicrobial stewardship programme, and our research involves collaborations with Clinical Pharmacology, Pharmacy, and clinical colleagues nationally and internationally.
Application of molecular diagnostics in routine diagnostic microbiology
 Recent advances in molecular diagnostic testing, such as PCR, have improved the sensitivity for detecting the aetiology of infections in a clinically relevant time frame.
Recent advances in molecular diagnostic testing, such as PCR, have improved the sensitivity for detecting the aetiology of infections in a clinically relevant time frame.
Canterbury Health Laboratories has been an early adopter of molecular diagnostics, and research has focused on the transition of these diagnostics into routine clinical use.
Zoonotic disease transmission
Around 60% of microorganisms causing human disease are passed between animals and humans (“zoonotic” pathogens). Changing farming practices in New Zealand are creating conditions promoting pathogen transfer between species.
In collaboration with colleagues at Massey University, we are studying the transmission of microorganisms between humans and animals, including antibiotic-resistant bacteria, with view to identifying interventions to control these infections.



