Friday 16 November 2018 8:54pm

Conjoined twins Nema and Dawa Pelden and their mother Bhumchu Zangmo. Photos: RCH Melbourne Creative Studio.
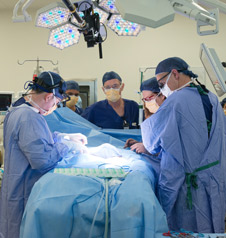
Otago graduate Dr Michael Nightingale was part of the surgical team which separated the twins at Royal Children’s Hospital in Melbourne last week.
A mix of relief, pride and protectiveness is how paediatric surgeon and Otago graduate Dr Michael Nightingale feels after being part of the team to successfully separate conjoined twins in Melbourne last week.
Dr Nightingale, who trained at the Otago Medical School, was one of four surgeons who completed the operation to separate twins Nima and Dawa Pelden, who were born in the Himalayan Kingdom of Bhutan in July 2017, and travelled with their mother Bhumchu Zangmo to the Royal Children’s Hospital (RCH) in Melbourne a month ago.
One of 18 in the operating theatre, Dr Nightingale helped separate the twins and then reconstruct Dawa’s abdomen.
“It’s a relief that it’s gone well, and I feel a lot of pride in the hospital and how we all worked together to make it possible,” he says.
“Primarily though I’m really pleased it went well for those two little girls and their family. I can’t imagine how stressful it must be to travel half way around the world to a new environment and entrust these people with your children, for a major operation.”
After the twins arrived in Melbourne, multiple teams of surgeons, anaesthetists, nurses and technicians worked with each other to plan and prepare for the operation. Dr Nightingale says the RCH is a big hospital which deals with a lot of difficult surgery.
“We’re fortunate to be able to work together in teams with lots of talented people.”
When patients come from overseas the clinicians often don’t have the information they need about their condition, so the first step is a critical assessment to work out what needs to be done, and the surgical plan follows from there. Retired members of staff were also consulted for their expertise.
“The hospital has a history of separating conjoined twins, so there is degree of ‘corporate knowledge’ which was very beneficial, especially for planning the anaesthetic.
“We also made sure that we had some juniors in the theatre, so they could learn and carry on the knowledge.”
Also present was Dr Karma Sherub, the only paediatric surgeon in Bhutan, who was flown out by the Children First Foundation. This meant he was able to give the surgeons advice during the operation on what processes he could manage in Bhutan, in terms of the care that would be available once the twins were back home.
"There is a surgical saying that goes plan well, cut well, then get well."
They had a run through the day before the surgery, deciding where to have the operating tables, how to set up the room for the scrub nurses and where the twins would be once separated.
“There is a surgical saying that goes plan well, cut well, then get well.”
On the day, everything to do with Nima was colour-coded green, while Dawa was red. The operation was also live-streamed to staff.
While the condition is rare, Dr Nightingale says the surgery was fairly straightforward and there were no surprises on the day. They knew the girls shared a liver, but had not been able to tell if the bowel was joined. Fortunately there was no significant attachment.
Despite having 18 people in the room (the twins were kept in the same theatre once separated), he didn’t find it greatly different from other operations.
“When I’m operating and concentrating on what I’m doing the noise around the sidelines disappears.”
The operation started around 8.30am and finished mid-afternoon, with a lot of time spent getting the anaesthetic right, and then positioning the twins on the operating table.
“Modern surgery is no longer about just the surgeon, it’s about the team. We have some incredibly talented people in different roles in the hospital, and we all work together to contribute to good outcomes.
“Because Nima and Dawa were lying in an unusual position, the work of the technician who was in charge of the padding around Nima and Dawa was crucial. The expertise people have in their roles is as important as the surgeon; I thought it was a really proud day because of how we all worked together.”
While it’s early days, he says so far the twins are making a great recovery and doing well, and if that continues they may be able to leave hospital in about two weeks.
"The world becomes more and more international, but a degree from Otago Medical School opens up doors."
Dr Nightingale has been amazed at the level of interest from media round the world.
“It’s been a little bit crazy. We’re very grateful for the interest in what we do, it’s really good to publicise some of the work the surgeons and nurses do, but we’re also conscious that we have two small girls and their mum taken from a very different environment and put into the glare of publicity – we’re quite protective of them.
”Having worked as a consultant at RCH since 2009, Dr Nightingale’s specialty is in paediatric oncology surgery.
He says he is “very proud” to have gone to Otago Medical School, and while initially he was attracted by the practical aspects of surgery, he was inspired as an undergraduate at the Department of Surgery, University of Otago, Christchurch, by Associate Professor Philip Bagshaw.
“He’s a highly skilled surgeon but it was his dedication to his patients, his great integrity and the endless time he had for students, including myself, that inspired me.”
He also says that when he was a postgraduate student, paediatric surgeon Professor Spencer Beasley was an important influence in his career.
“He had so much enthusiasm for the care of children and was such fun to work with in surgery.”
His best friends are all people he met while at Knox College and during medical school, and he’s trying to convince his own children to go to Otago.
“The world becomes more and more international, but a degree from Otago Medical School opens up doors.”
