Professor Stephen Robertson, Group Leader

Professor Stephen Robertson.
Email stephen.robertson@otago.ac.nz
Stephen Robertson is the Cure Kids Professor of Paediatric Genetics at the University of Otago in Dunedin. He graduated in Medicine in 1990 and specialised in Paediatrics and Genetics after training at various hospitals in greater Auckland and at the Victorian Clinical Genetics Service in Melbourne from 1997–1999. From 1995–1996, he was Chief Resident of Starship Children's Hospital in Auckland. From 1999–2002, Stephen was Nuffield Medical Fellow at St Catherine's College, Oxford University, studying the genetic determinants of congenital malformations in children. This work was conducted in the laboratory of Professor Andrew Wilkie at the Weatherall Institute of Molecular Medicine. Since relocated to Dunedin in 2002 he has developed strong research themes in the area of paediatric genetics that has focused on conditions that result in malformations, neurodevelopmental disability and Māori genomics. He remains an active clinical geneticist attached to Genetic Health Services New Zealand as well as teaching into the Genetics Teaching Programme, undergraduate and postgraduate medical programmes and Medical Laboratory Science.
View Professor Stephen Robertson's staff profile
The Curekids Chair in Child Health Research
![]()

Curekids Fundraiser.
The Child Health Research Foundation (subsequently re-branded as Curekids) launched an initiative in 2002 to establish a chair at the University of Otago that was dedicated to aspects of child health research. A large number of corporate organisations and private individuals contributed to the establishment of the position. Most notably, four men from Queenstown – Graham Smolenksi, Jeff Turner, Wayne Cafe, and Fraser Skinner – initiated an international ski endurance event – The 50k of Coronet – over five successive years from 2000–2004 to contribute over $1 million to the fund. Professor Robertson was appointed as the Inaugural Curekids Professor in late 2002 and established the Clinical Genetics Group. In 2006, in collaboration with the Government's Partnerships in Excellence Programme and the University's Leading Thinkers Programme, the Curekids Chair in Child Health Research was established in perpetuity.
Read more about the Curekids Chair in Child Health Research at the Curekids website
Current staff
Zandra Jenkins
Research Fellow
Email zandra.jenkins@otago.ac.nz
 __STH__I began my research studying the molecular genetics of wool at the AgResearch Molecular Biology Unit, University of Otago, completing my doctorate in 1998. I went on to carry out postdoctoral research at the Department of Cell and Molecular Biology, Uppsala University Sweden (1998–2000) studying protein translation. I continued this research at the Childrens Hospital Oakland Research Institute, USA (2000–2002), in addition to studying the regulation of iron homeostasis in patients with sickle cell anaemia and β-thalassemia. Returning to New Zealand in 2003, I joined the Clinical Genetics Group as a Research Fellow.
__STH__I began my research studying the molecular genetics of wool at the AgResearch Molecular Biology Unit, University of Otago, completing my doctorate in 1998. I went on to carry out postdoctoral research at the Department of Cell and Molecular Biology, Uppsala University Sweden (1998–2000) studying protein translation. I continued this research at the Childrens Hospital Oakland Research Institute, USA (2000–2002), in addition to studying the regulation of iron homeostasis in patients with sickle cell anaemia and β-thalassemia. Returning to New Zealand in 2003, I joined the Clinical Genetics Group as a Research Fellow.
Emma Wade
Postdoctoral Fellow
Email emma.wade@otago.ac.nz
 Emma completed her undergraduate degree in genetics at the University of York in 2010. She spent the next two years working in the clinical genetics group at Manchester University as a research assistant, studying the genetic cause of glaucoma.
Emma completed her undergraduate degree in genetics at the University of York in 2010. She spent the next two years working in the clinical genetics group at Manchester University as a research assistant, studying the genetic cause of glaucoma.
In 2013 she moved to the University of Otago to complete her PhD with Prof. Stephen Robertson in the Department of Women's and Children's Health. Her PhD research focused on the genetic cause of rare, childhood bone diseases and how these genetic mechanisms contribute to how the skeleton senses force. Her PhD uncovered mutations in two genes which lead to an exciting hypothesis and ultimately a Marsden funded project for the Clinical Genetics group.
She is now employed as a postdoctoral fellow pursuing a project which has grown out of her PhD: trying to untangle the signalling pathways which maintain skeletal homeostasis.
Ben Halliday
Postdoctoral Fellow
Email benjamin.halliday@otago.ac.nz
 I completed my BSc(Hons) in 2016, exploring the genetic drivers of childhood kidney cancers. Through this project I developed a passion for bioinformatics, particularly in the application of genome sequencing techniques to explore rare disease genetics.
I completed my BSc(Hons) in 2016, exploring the genetic drivers of childhood kidney cancers. Through this project I developed a passion for bioinformatics, particularly in the application of genome sequencing techniques to explore rare disease genetics.
In 2017, I began my PhD in the Laboratory for Genomic Medicine. My doctoral research focused on the genomic investigation of patients with brain malformations, providing diagnostic answers for patients and their families, as well as improving understanding of the genetic pathways critical for brain development.
I am now a Postdoctoral Fellow in the Laboratory for Genomic Medicine, and contribute to several ongoing projects in the lab. My main project involves assessing the appropriateness of first-tier genomic diagnostic tools in New Zealand, and investigating why these tools have reduce performance in Māori and other Pacific Peoples.
Elizabeth Goodin
Assistant Research FellowEmail liz.goodin@otago.ac.nz
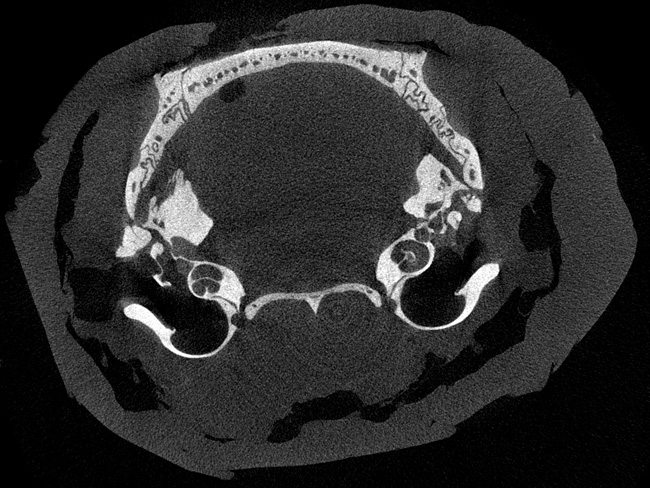
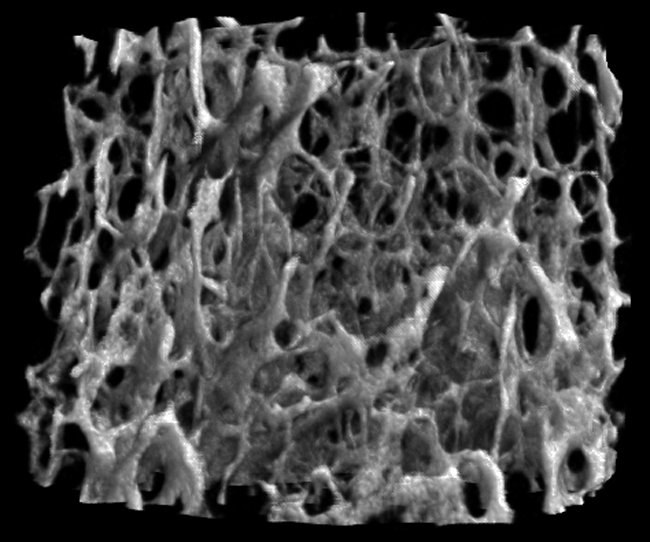
 I joined the Clinical Genetics Group as a Research Technician in 2019, working mainly with mouse models which help us learn more about skeletal development. One interesting technique I use is Micro CT, which is 3D x-ray scanning of small (micro) structures, in our case mouse bones. These scans allow us to compare bones between groups of mice with or without a particular genetic change and investigate how certain genes might be important in bone structure.
I joined the Clinical Genetics Group as a Research Technician in 2019, working mainly with mouse models which help us learn more about skeletal development. One interesting technique I use is Micro CT, which is 3D x-ray scanning of small (micro) structures, in our case mouse bones. These scans allow us to compare bones between groups of mice with or without a particular genetic change and investigate how certain genes might be important in bone structure.
Previously, from 2017–2019, I carried out work in our lab on behalf of the world famous Dunedin Longitudinal Study, which studies human health, development and behaviour. In this role, I processed and catalogued past and present study member samples, including DNA. Prior to that, I completed a master's degree with the Robertson group, taking a close look at the gene MET, which is important in a bone disease called Osteofibrous Dysplasia (OFD). Among other techniques, I used specially designed antisense oligonucleotides to target certain RNA sites in cells, in search of what might regulate the differential processing of this gene to cause disease.
Tim Morgan
Research Technician
Email tim.morgan@otago.ac.nz
 I completed my MSc in Biochemistry in Professor Julian Eaton-Rye's lab in 2000, working on photosysthesis research. From there, I started working in Professor Robin Old's lab on bipolar disorder. Then I moved to Professor Stephen Robertson's new lab in 2003, working mainly with Filamin A, Filamin B and WTX.
I completed my MSc in Biochemistry in Professor Julian Eaton-Rye's lab in 2000, working on photosysthesis research. From there, I started working in Professor Robin Old's lab on bipolar disorder. Then I moved to Professor Stephen Robertson's new lab in 2003, working mainly with Filamin A, Filamin B and WTX.
Professor Mac Gardner
Adjunct Professor
Email macgardner@gmail.com
 Professor Gardner is a semi-retired medical geneticist. He is an Otago graduate, who was previously a member of the Paediatrics Department (1977–1993), before moving to the Genetic Service based at the Royal Children's Hospital in Melbourne (1993–2007). He has broad clincal interests, with a particular focus on inherited cerebellar ataxias and chromosomal disorders. He co-authors the textbook 'Chromosome Abnormalities and Genetic Counseling', and is presently preparing a 4th edition. He shares a spot in Professor Stephen Robertson's office in the Hercus Building.
Professor Gardner is a semi-retired medical geneticist. He is an Otago graduate, who was previously a member of the Paediatrics Department (1977–1993), before moving to the Genetic Service based at the Royal Children's Hospital in Melbourne (1993–2007). He has broad clincal interests, with a particular focus on inherited cerebellar ataxias and chromosomal disorders. He co-authors the textbook 'Chromosome Abnormalities and Genetic Counseling', and is presently preparing a 4th edition. He shares a spot in Professor Stephen Robertson's office in the Hercus Building.
PhD students
Annika Sjoeholm
PhD student
 Dr Annika Sjoeholm is an advanced trainee Paediatric registrar with the Royal Australasian College of Physicians. Annika completed her undergraduate medical training at the Dunedin School of Medicine, University of Otago in 2011. She holds a first class BMedSc(Hons) degree in neuroendocrinology (thesis on changes in the maternal brain from the Centre of Neuroendocrinology, Otago University). Annika began her PhD in human molecular genetics in 2017, supported by a Lady King Scholarship. Beyond her PhD she is engaged with the Clinical Genetics group in the translation of a rare disease gastrointestinal phenotype into a common disease mechanism. Annika particularly enjoys developmental paediatrics and clinical genetics, and bridging the gap between lab work and clinical work.
Dr Annika Sjoeholm is an advanced trainee Paediatric registrar with the Royal Australasian College of Physicians. Annika completed her undergraduate medical training at the Dunedin School of Medicine, University of Otago in 2011. She holds a first class BMedSc(Hons) degree in neuroendocrinology (thesis on changes in the maternal brain from the Centre of Neuroendocrinology, Otago University). Annika began her PhD in human molecular genetics in 2017, supported by a Lady King Scholarship. Beyond her PhD she is engaged with the Clinical Genetics group in the translation of a rare disease gastrointestinal phenotype into a common disease mechanism. Annika particularly enjoys developmental paediatrics and clinical genetics, and bridging the gap between lab work and clinical work.
Amy Jones
PhD student
 I completed my BSc (Hons) in 2019 investigating Pseudomonas aeruginosa, the bacteria responsible for the majority of lung infections in cystic fibrosis patients.
I completed my BSc (Hons) in 2019 investigating Pseudomonas aeruginosa, the bacteria responsible for the majority of lung infections in cystic fibrosis patients.
In 2020 I began my PhD in the Clinical Genetics group. My project aims to understand how metabolism contributes to neurodevelopment. Specifically, I will be investigating the metabolite glutamine, one of the most abundant amino acids in the human body. My work utilises genetic and biochemical techniques to understand how glutamine influences neurodevelopment.
Other students
Recent photos of the Clinical Genetics Group

2022: Left to right: Back row: Ben Halliday (Postdoctoral Fellow), Stephen Robertson (Group leader), Tim Morgan (Laboratory Technician), Kam Salt (PGDipSci). Front row: Emma Wade (Postdoctoral Fellow), Amy Jones (PhD student), Hayley Gibson (BMedSc(Hons) Student), Elizabeth Goodin (Assistant Research Fellow), Padmini Parthasarathy (Assistant Research Fellow), Zandra Jenkins (Research Fellow).

2018: Left to right: Back row: Wenhua Wei (Senior Research Fellow), Kaya Fukushima (Summer Student), Sean Driver (Masters student), Emma Wade (Postdoctoral Fellow), Stephen Robertson (Group leader), Ben Halliday (PhD student), Tim Morgan (Laboratory Technician). Front row: Annika Sjoeholm (PhD student), Zandra Jenkins (Research Fellow), Hui Peng (Visiting PhD Scholar), Padmini Parthasarathy (Assistant Research Fellow).