CRITICAL-ACS: Using CT to reduce invasive coronary angiograms in heart attacks
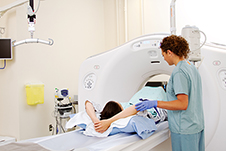 This study is testing the ability of non-invasive CT scans to reduce the need for traditional coronary angiograms ('catheter tests') to look at the heart arteries of people with a suspected heart attack.
This study is testing the ability of non-invasive CT scans to reduce the need for traditional coronary angiograms ('catheter tests') to look at the heart arteries of people with a suspected heart attack.
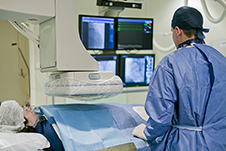
Both tests are safe and effective ways to look at the heart arteries and there are advantages and disadvantages to both. Traditional coronary angiograms allow blocked arteries to be opened and treated with 'stents' during a single procedure but can cause some discomfort as a tube ('catheter') needs to be threaded up from the risk or groin to reach the heart. CT scans are less invasive and provide similar information to catheter-based angiograms. For about 1 in 3 patients this would be the only test required but if blockages are found, patients would require the traditional coronary angiogram to allow these to be treated. Importantly, whilst CT scans are available at nearly all NZ hospitals treating heart attacks, coronary angiograms can only be performed at the larger centres so many patients need to be transferred between hospitals for this.
Participants involved in this study will have been identified when their treating doctor suspects they have had a heart attack and wants to look at the heart arteries to confirm this. After consenting to participate in the study, patients will be randomly allocated to undergo either the CT scan or the traditional coronary angiogram as the first test. Every participant will continue to receive all the usual treatments for their heart and if the CT scan identifies problems that may need treatment these patients will still need to undergo the catheter-based test. We expect to reduce the need for the more invasive procedure by about one third.
For more information about the study, please watch this short animation:
For further information, you can speak with a Research Nurse:
Tel +64 3 364 1759
Txt +64 21 0836 7936
Hauora Manawa/Heart Health: The Community Heart Study
There is a major disparity between Māori and non-Māori in cardiovascular mortality.
Few studies exist on the prevalence and incidence of cardiovascular disease in the Māori community. Our research aims to collect information on:
- Current levels of established heart disease
- Previously undiagnosed diabetes
- Cardiovascular disease and their risk factors in randomly-selected population samples
The samples groups are:
- Ngāti Kahungunu ki Wairoa in Hawkes Bay
- Mana Whenua ki Waitaha in Canterbury
- A non-Maori control group in Canterbury
Find out more about the Hauora Manawa/Heart Health: The Community Heart Study
CNP – what role does it play in combatting Arteriosclerosis?
We are studying a hormone called CNP, or C-type Natriuretic Peptide and the role it may play in combatting the hardening of the arteries.
What are Natriuretic Peptides?
- They are a well family of heart hormones which respond to major heart events, like a heart attack or heart failure.
- The family consists of 3 related hormones: Atrial natriuretic peptide (ANP), B-type natriuretic peptide (BNP) and CNP.
What is CNP?
- CNP is expressed in a wide range of tissues, including those outside the cardiovascular system
- While ANP and BNP are known to be cardio-protective, the effects of CNP are not well understood.
Our researchers are investigating CNP, its relationship with the heart hormones ANP and BNP and the role CNP plays in humans. The team is also working in collaboration with colleagues from around New Zealand and the United States on CNP's role in skeletal growth, pregnancy and in nerve tissue.
Unlike ANP and BNP, CNP appears to be more active within the walls of blood vessels where it is thought to protect against the development of hardening of the arteries (arteriosclerosis).
Professor Espiner and Dr Prickett currently have grants from the National Heart Foundation and Lottery Health to study changes in blood and tissue levels of CNP during the build-up of vascular plaque that eventually leads to coronary artery disease.
Our researchers are also trying to evaluate whether standard cholesterol lowering drug treatments (Statins) raise the blood level of CNP, and if so, could this be used to determine the state of health of the blood vessels. There is currently no marker to evaluate the health of blood vessels which is crucial for a healthy heart.
It is envisaged that these studies could lead to new treatments for one of the most common forms of heart disease in the western world.
New Projects
Information on all of our new projects coming soon!
